
Lymphatic drainage relates to how the body manages fluid, waste, and immune activity each day. When this system slows, the effects often appear quietly and progress over time. Many people notice discomfort without linking it to fluid circulation beneath the skin. These changes affect energy, appearance, and physical ease in ways that feel familiar but hard to explain. Recognizing these patterns helps clarify when lymphatic drainage support becomes relevant.
Lymphatic drainage refers to the movement of lymph fluid through vessels and nodes. This bodywide process removes waste while maintaining tissue balance. Unlike blood flow, lymph movement depends on breathing and muscle activity. When flow slows, fluid remains where it should not.
Natural lymphatic drainage slows when daily movement decreases and stress increases. Sedentary routines limit muscle contractions that push lymph forward. Shallow breathing reduces the diaphragm motion needed for fluid transport. Dehydration thickens lymphatic fluid, making movement more difficult. Over time, these factors combine and strain circulation. This cumulative strain rarely causes sudden symptoms.
Lymph congestion builds quietly because it lacks pain receptors early on. Swelling and pressure feel mild at first and fluctuate. Many people attribute changes to aging or routine stress. The body adapts temporarily, masking the issue. Over months, compensation becomes less effective. Symptoms then feel more persistent and noticeable.
Impaired lymphatic flow manifests as physical patterns that tend to recur rather than resolve. These signals often appear across multiple body systems, making them easy to overlook or misinterpret. Discomfort, swelling, or fatigue may seem unrelated at first, yet they often share the same underlying cause. Understanding these indicators provides context for the following reasons and clarifies why lymphatic drainage support is relevant.
Persistent swelling reflects trapped fluid that the lymphatic system has not cleared. This swelling often feels dense rather than soft. It may improve overnight but return daily. Areas affected usually follow gravity.
Lymphatic-related limb swelling appears in the arms or legs without injury. The skin may feel tight or heavy in the afternoon. Socks or sleeves may leave deeper impressions. Elevation provides temporary relief but does not resolve the issue. Movement may feel restricted rather than painful. This pattern suggests reduced fluid clearance.
Facial swelling often shows around the eyes or jaw after waking. Neck fullness may limit comfortable head movement. The sensation feels pressurized rather than inflamed. Sinus congestion may accompany these changes. Symptoms often recur despite rest or hydration. This consistency points toward lymph stagnation.
Abdominal swelling tied to lymph flow feels firm after meals. The pressure differs from gas-related bloating. Clothing may feel uncomfortable even with light eating. Digestive changes alone rarely correct this issue. Lymph vessels around the gut may hold excess fluid. This abdominal pressure often worsens later in the day.
Lymph congestion often produces physical and mental fatigue. The body expends more energy managing the buildup of waste. Rest may not restore usual vitality. This fatigue feels weighted rather than sleepy.
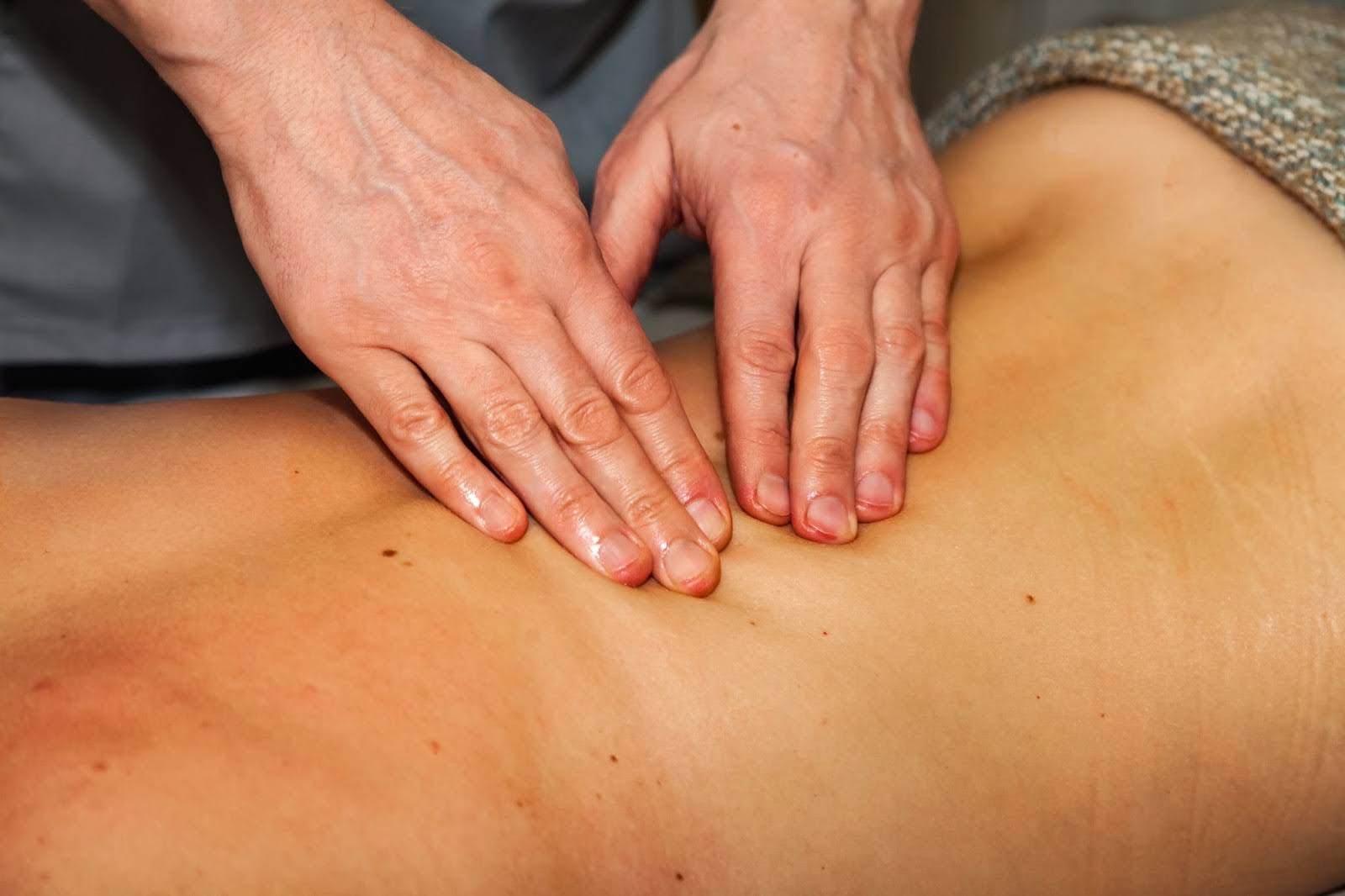
Lymph-related fatigue persists despite adequate sleep. Energy drops appear earlier during daily routines. Mental focus may feel dulled or inconsistent. Toxin buildup increases internal workload. The body works harder to maintain balance. This effort drains energy steadily.
Movement may feel laborious without intense exertion. Legs or arms may feel dense instead of flexible. Muscles tire quickly during routine tasks. Stretching offers brief relief. The heaviness returns soon after stopping. This recurring sensation reflects fluid retention.
The lymphatic system supports immune defense by transporting fluid. When drainage slows, immune efficiency declines. Minor illnesses may appear more often. Recovery may feel incomplete.
Recurring colds often result from sluggish lymph flow. Sinuses rely on lymph drainage to reduce pressure. Congestion may linger longer than expected. Symptoms may cycle without full relief. Stress often worsens these patterns. This recurrence suggests impaired fluid clearance.
Skin health reflects internal lymph function. Slow drainage allows bacteria to linger. Minor cuts may be prone to inflammation easily. Rashes may reappear in similar areas. Healing takes longer than usual. This sensitivity signals immune strain.
Healing depends on efficient lymphatic drainage. When flow slows, inflammation lingers. Injuries may resolve unevenly. Discomfort may persist beneath healed skin.
Bruises may remain visible for extended periods. Swelling around injuries may feel firm. Tenderness may outlast visible healing. Fluid clearance slows tissue repair. Repeated injuries may compound inflammation. This delayed recovery reflects lymph congestion.
Inflammation may feel warm or pressurized without injury. Sensations may shift locations unpredictably. Anti-inflammatory methods may help briefly. Relief rarely lasts without improved drainage. This pattern suggests internal fluid buildup. Ongoing inflammation stresses surrounding tissues.
The digestive system relies on lymph vessels to transport fats and waste products. When drainage slows, discomfort follows meals. Symptoms often feel physical rather than dietary. Digestive balance becomes harder to maintain.
Lymph-related bloating feels heavy and firm. Pressure increases even after small meals. Posture changes offer limited relief. The abdomen may remain distended for hours. This discomfort differs from gas buildup. Fluid retention often causes this pressure.
Waste removal slows when lymph flow decreases. Bowel habits may become inconsistent. Toxins may recirculate instead of exiting. Fatigue or skin changes may follow. Hydration alone rarely resolves this pattern. Improved drainage often supports regularity.
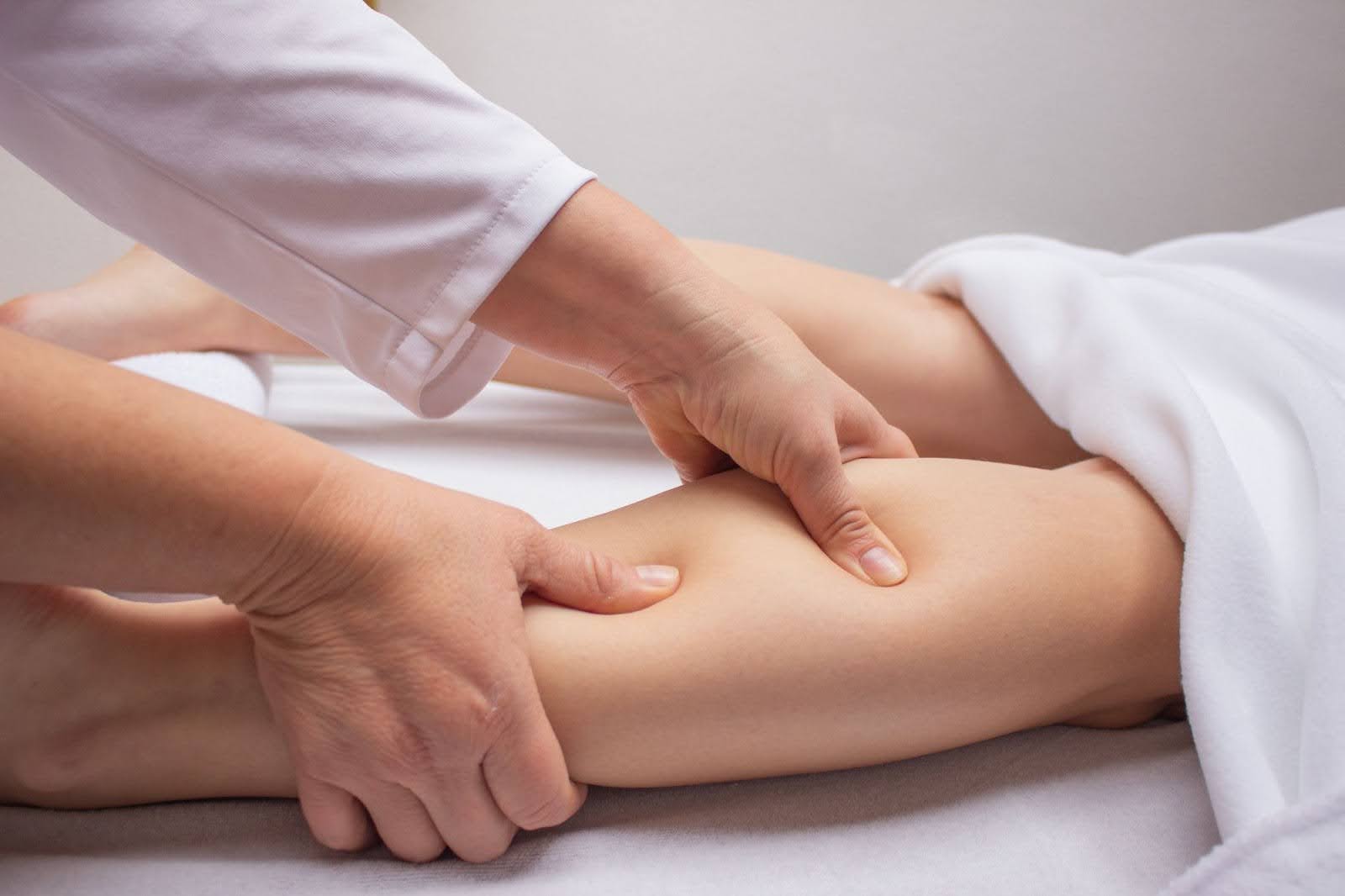
Skin reflects internal circulation and waste removal. Lymph congestion alters the appearance and feel of the skin. Topical care may offer limited improvement. Changes often develop gradually.
Cellulite increases when fluid traps beneath the skin layers. Exercise may improve tone without smoothing texture. Affected areas may feel tender. Thighs and hips often show changes first. This texture reflects fluid stagnation. Fat alone does not explain this pattern.
Skin may lose brightness with slow drainage. Redness or irritation appears more easily. Acne may recur in similar spots. Products may cause sensitivity unexpectedly. Healing slows after flare-ups. These signs mirror internal congestion.
Lymph congestion produces diffuse discomfort rather than sharp pain. Sensations often feel pressurized or aching. Symptoms may shift throughout the body. Comfort may decline gradually.
Lymph nodes may feel sore without illness. The neck and underarms are often sensitive. Pressure increases during stress. Tenderness may fluctuate daily. Temporary relief often occurs with rest. Persistent soreness suggests restricted flow.
Fluid buildup in the facial pathways can trigger pressure headaches. Pain often centers behind the eyes. Morning symptoms feel stronger. Weather changes may worsen discomfort. Medication offers limited relief. Drainage improvement often reduces pressure.
Daily habits influence lymphatic efficiency. Small choices accumulate over time. Modern routines often limit natural drainage. Awareness helps reduce strain.
Extended sitting reduces muscle-driven fluid movement. Swelling increases during travel or desk work. Stiffness develops without activity breaks. Brief movement helps temporarily. Baseline swelling may rise over time. Consistent motion supports flow.
Stress shortens breathing patterns. Reduced diaphragm motion limits lymph propulsion. Muscle tension narrows fluid pathways. Emotional strain often mirrors physical congestion. Relaxation supports drainage naturally. This connection often goes unnoticed.
Lymph fluid thickens without adequate hydration. Thick fluid moves inefficiently. Poor nutrition affects vessel health. Inflammation increases with processed foods. These factors burden circulation. Balance supports smoother flow.
Lymphatic drainage massage is a manual technique designed to encourage the movement of lymph fluid. This approach works with the body’s natural pathways rather than forcing deep pressure. It directly addresses many signs discussed earlier, including swelling, heaviness, and fatigue. The method focuses on restoring smoother circulation where stagnation has developed.
Lymphatic drainage massage uses slow, rhythmic strokes that follow the direction of lymph vessels. Pressure is kept low to prevent the collapse of delicate lymphatic channels. This technique stimulates lymph nodes and encourages fluid to move toward drainage points. As fluid clears, tissues often feel less tight or pressurized. Many people notice improved comfort shortly after sessions. These effects align with the symptoms described earlier, including swelling, congestion, and heaviness.
Lymphatic drainage massage becomes relevant when symptoms persist despite lifestyle adjustments. Swelling that returns daily often responds well to guided fluid movement. Fatigue linked to congestion may ease as waste removal improves. Digestive pressure may reduce as abdominal lymph flow increases. Skin texture and sensitivity often improve gradually with consistent care. This supportive approach complements the body’s natural processes rather than overriding them.
A lymphatic drainage session feels gentle and controlled rather than intense or forceful. The practitioner uses slow, repetitive movements that follow established lymph pathways. Pressure stays light to protect superficial vessels near the skin. Sessions often begin near the neck to clear central drainage points. Many people report a calming effect as the nervous system settles. This experience aligns with the article’s focus on reducing congestion without causing strain.
Lymphatic drainage care offers a practical way to respond when the body signals overload through swelling, fatigue, or pressure. Addressing lymphatic flow helps the body clear what no longer serves it, rather than forcing constant compensation. With proper support, tissues regain ease, energy feels steadier, and recurring discomfort becomes less dominant. Choosing lymphatic drainage care reflects an informed decision to support long-term comfort through intentional, body-aware action.
Stay informed about lymphatic health, advanced treatments, and expert guidance on the Naples Laser & Skin Aesthetics blog.
%402x.svg)

.png)
3641 10th St N Suite B, Naples, FL 34103