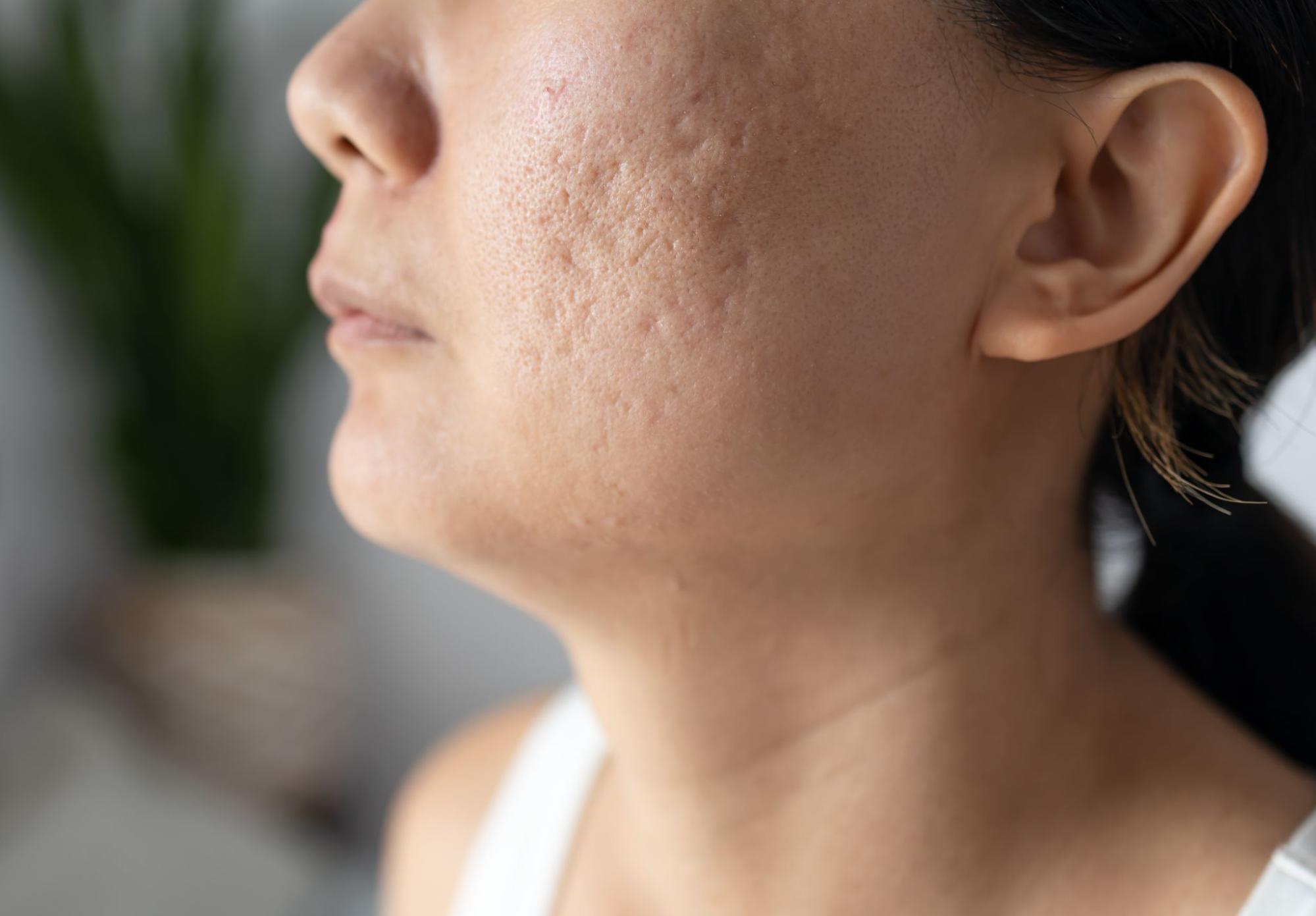
Acne scarring often remains long after active breakouts resolve, creating lasting frustration for many people. These skin changes develop when inflammation disrupts the normal healing process. Some scars affect only skin color, while others permanently alter texture and depth. Results vary widely because scar type, skin biology, and treatment timing differ. Learning how to get rid of acne scarring begins with understanding what causes scars and how skin repairs itself.
Acne scarring refers to permanent skin changes caused by damaged collagen during acne healing. This condition forms when inflammation penetrates deeper skin layers. The body attempts repair, but uneven collagen production creates visible texture differences. Understanding the origin of scarring helps guide realistic treatment decisions.
Acne marks are surface-level color changes left after pimples heal. These marks appear red, brown, or purple depending on skin tone. True acne scars involve physical changes in skin texture and depth. This distinction matters because marks often fade naturally over time. Scars require targeted treatment to improve appearance. Identifying the difference prevents unnecessary product use and frustration.
Inflammation drives scar formation more than acne size alone. When swollen pores rupture, the surrounding tissue sustains damage. The skin responds by producing collagen to repair itself. Too little collagen causes depressions, while excess creates raised scars. Longer inflammation increases the risk of uneven healing. Managing inflammation early reduces the likelihood of scarring.
Genetics influence how skin heals after acne. Some people naturally produce more or less collagen. Skin thickness and oil production also affect scarring patterns. Deeper skin tones may develop darker marks more easily. Frequent breakouts increase cumulative tissue damage. Personalized care improves long-term outcomes.
Acne scars vary widely in shape, depth, and severity. Identifying scar type determines effective treatment options. Some scars respond to topical care, while others require clinical procedures. Clear classification prevents unrealistic expectations.
Ice pick scars appear narrow and deep, resembling puncture marks. These scars form when inflammation destroys collagen deep within pores. Topical treatments rarely significantly improve this scar type. Professional procedures stimulate deeper collagen repair. Improvement occurs gradually rather than instantly. Proper diagnosis guides appropriate treatment selection.
Boxcar scars appear wider with defined edges. Rolling scars create uneven, wave-like skin texture. Both result from collagen loss during healing. These scars often respond to resurfacing treatments. Repeated stimulation encourages smoother skin over time. Gradual improvement remains the norm.
Raised scars develop when excess collagen forms during healing. Keloids may extend beyond the original acne site. These scars commonly appear on the jawline or chest. Treatment focuses on reducing collagen overproduction. Early management improves control and appearance. Professional evaluation remains important.
Pigmentation affects skin color without altering texture. Structural scars change skin depth and surface. This distinction influences treatment choice greatly. Brightening products fade pigmentation over time. Structural scars require collagen remodeling. Correct identification saves time and expense.
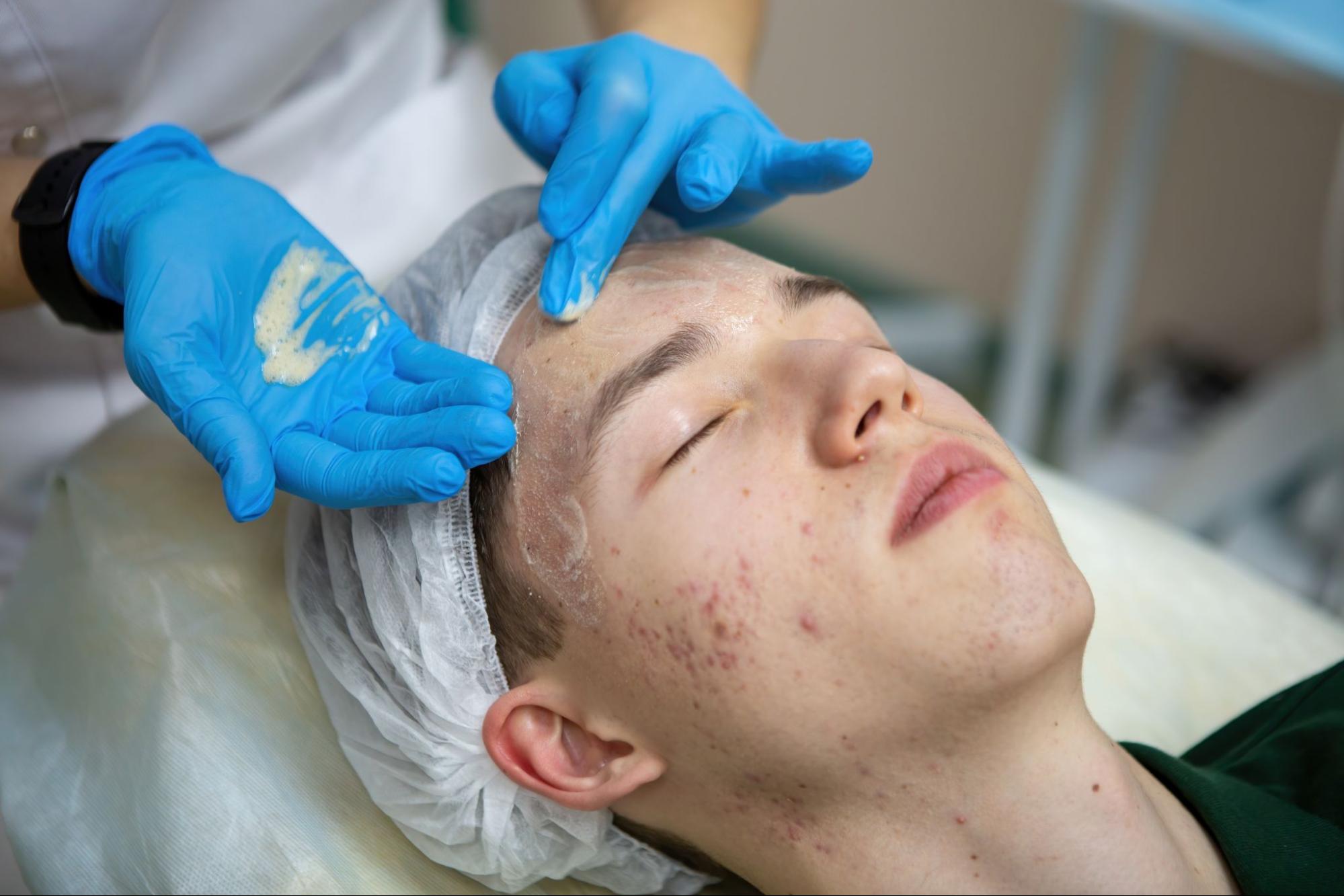
Daily skincare plays a role in how scars fade over time. Gentle routines protect the skin barrier during healing. Consistency matters more than product quantity. Small habits accumulate visible benefits.
Gentle cleansing removes oil without disrupting healing. Harsh cleansers increase irritation and inflammation. This skincare step supports a stable skin barrier. Lukewarm water reduces sensitivity during washing. Overcleansing delays repair and worsens texture. Balanced cleansing promotes recovery.
Sun exposure darkens healing scars significantly. Ultraviolet rays stimulate pigment production in damaged skin. Daily sunscreen prevents long-term discoloration. Broad-spectrum formulas protect against UVA and UVB damage. Reapplication maintains consistent coverage. Sun protection improves treatment results.
Moisturizing supports collagen repair and elasticity. Hydrated skin heals more efficiently. Ceramides and humectants reinforce the skin barrier. This hydration step reduces irritation from active treatments. Skipping moisturizer increases the risk of sensitivity. Consistent hydration supports resilience.
Skin barrier health refers to the outer layer of the skin that protects against moisture loss and irritation. This barrier controls inflammation, hydration, and the efficiency of healing. When the barrier weakens, scar repair slows noticeably. Supporting barrier strength improves treatment response and overall skin resilience.
A weakened skin barrier allows moisture to escape rapidly. This dehydration disrupts cellular repair processes. Inflammation increases when irritants penetrate damaged skin. This inflammatory state impairs collagen repair. Treatments become less effective under these conditions. Healing appears slower and more uneven.
Excessive exfoliation and active ingredients damage the barrier. This overuse increases sensitivity and redness. Scar tissue responds poorly when irritation persists. Collagen stimulation becomes inconsistent under stress. Reducing treatment frequency often improves results. Balanced routines protect long-term progress.
Strong barriers tolerate microneedling, retinoids, and PRP more effectively. Recovery time is shorter when the skin remains hydrated and intact. This resilience allows consistent treatment scheduling. Reduced irritation improves adherence to care plans. Better tolerance supports cumulative improvement. Barrier care directly influences outcomes.
Barrier support includes proper cleansing, moisturizing, and sun protection. Ingredients like ceramides reinforce structural integrity. This supportive care reduces treatment setbacks. Hydrated skin responds more predictably to stimulation. Consistent barrier repair stabilizes progress. Strong foundations enhance visible improvement.
Topical treatments help improve mild-to-moderate scarring. Results depend on scar type and consistency of use. Patience remains necessary for visible change. Ingredient selection matters greatly.
Retinoids increase cell turnover and collagen production. These compounds gradually smooth skin texture. Initial dryness may occur during adjustment periods. Gradual introduction reduces irritation risk. Sunscreen supports safe retinoid use. Long-term consistency yields improvement.
Chemical exfoliants remove damaged surface cells. These acids improve tone and texture evenly. Overuse causes irritation and delays healing. Controlled frequency protects skin balance. Professional guidance improves safety. Gentle exfoliation supports gradual refinement.
Brightening ingredients reduce post-acne discoloration. Niacinamide and azelaic acid calm inflammation. These formulas support even skin tone. Results appear slowly with consistent use. Combining brighteners with sunscreen enhances fading. Balanced formulas reduce irritation risk.
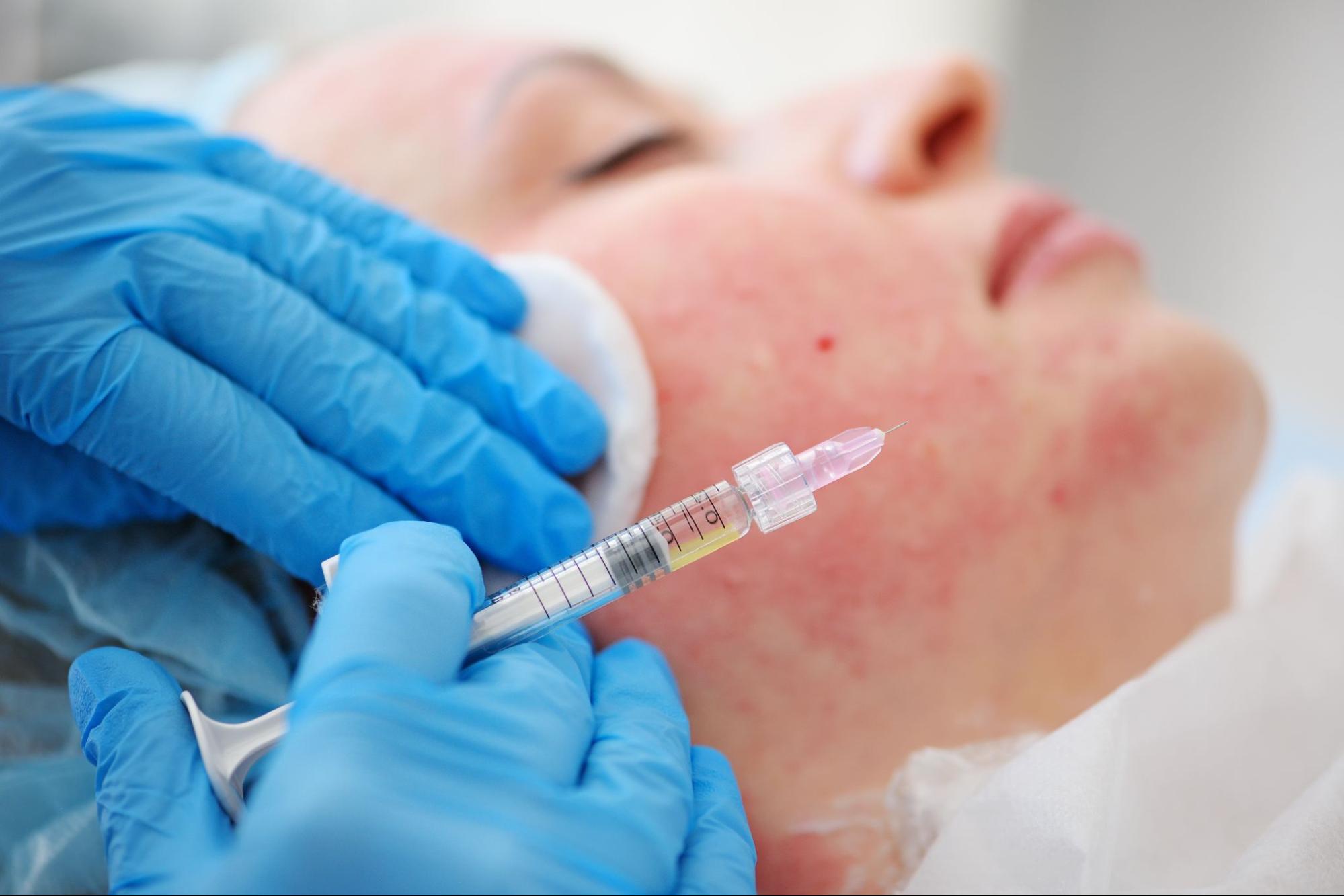
Clinical procedures address scars beyond the reach of topical treatments. These treatments stimulate collagen production directly. Results vary by scar depth and skin response. Professional evaluation guides selection.
Microneedling improves acne scars by creating controlled micro-injuries in the skin. This treatment activates the body’s natural collagen and elastin production. The process helps soften the uneven texture caused by atrophic scars. Providers typically recommend a series of sessions for visible improvement. Recovery time remains short, with mild redness resolving quickly. Gradual collagen rebuilding leads to smoother skin over time.
Laser treatments address acne scars by targeting damaged skin layers with focused energy. This approach stimulates collagen production while resurfacing uneven texture. Different laser types treat scars of varying depths and skin tones. Treatment plans depend on scar severity and skin sensitivity. Downtime ranges from minimal to moderate based on the laser used. Results develop progressively as the skin repairs itself.
This treatment concentrates growth factors that stimulate healing in scarred tissue. Providers often pair PRP with microneedling or laser treatments to improve results. The microneedling process creates channels that allow PRP to penetrate deeper into the skin. Clinical observations from dermatology practices show improved texture and elasticity with combined treatments. Results appear gradually as collagen rebuilds over several weeks.
Acne scar age refers to how long scar tissue has been present in the skin. This factor influences collagen structure, blood supply, and treatment responsiveness. Newer scars behave differently from older scars at a biological level. Recognizing scar age helps set realistic expectations and guides treatment planning.
Newer acne scars retain higher cellular activity and better circulation. This biological state allows collagen to respond more readily to stimulation. Treatments such as microneedling and PRP show faster improvement at this stage. Inflammation remains more reversible in recent scars. Skin remodeling processes activate more efficiently. Earlier intervention shortens visible recovery timelines.
Older acne scars develop rigid collagen fibers over time. This structure limits flexibility and slows remodeling. Blood flow within the scar tissue also decreases. These changes reduce responsiveness to single treatments. Layered approaches become necessary for visible improvement. Progress occurs gradually rather than dramatically.
Treatment planning changes when scar age is taken into account. Newer scars often respond to fewer sessions and gentler methods. Older scars benefit from combined modalities targeting deeper layers. Providers may adjust energy levels or session spacing. This strategy improves safety and effectiveness. Tailored plans reduce unnecessary treatments.
Prevention reduces the need for correction later. Managing acne carefully protects skin structure. Gentle responses limit lasting damage. Proactive habits preserve texture.
Picking ruptures follicles and deepens inflammation. This behavior increases scar risk dramatically. Healing slows when irritation persists. Bacteria from the hands worsen the infection. Leaving blemishes alone protects tissue. Patience prevents damage.
Consistent acne control reduces inflammation cycles. Controlled breakouts heal more evenly. Delayed care increases scarring risk. Tailored routines improve outcomes. Professional input enhances control. Prevention supports clarity.
Trained providers assess patterns of inflammation and risk factors. This evaluation allows targeted treatment adjustments. Early clinical care reduces the risk of repeated tissue injury. Consistent monitoring improves long-term skin outcomes. Informed intervention protects skin structure.
Acne scarring improves when consistent care replaces trial and error. Skin responds best to treatments grounded in biology, not trends. Progress occurs when methods align with scar type, skin condition, and healing capacity. A disciplined approach builds visible improvement and restores confidence over time.
Explore expert insights on skin health and advanced treatments on the Naples Laser & Skin Aesthetics blog, where informed care meets real results.
%402x.svg)

.png)
3641 10th St N Suite B, Naples, FL 34103