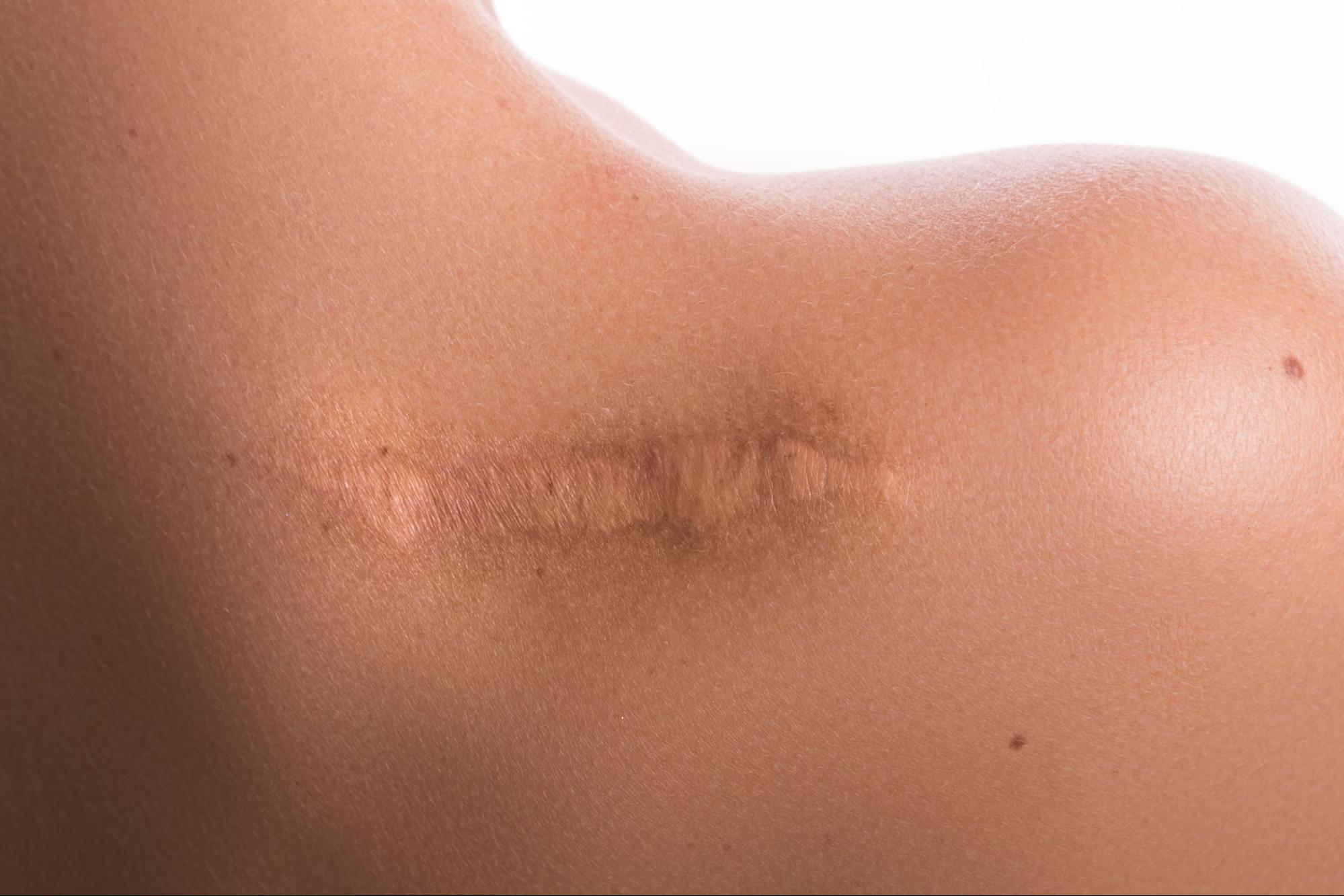
Many people live with skin scarring long after wounds appear to heal. Acne breakouts, injuries, burns, and surgery often leave visible marks that change skin texture. These marks can affect confidence because scars remain noticeable in daily life. Skin repair naturally protects the body, yet the healing process rarely restores the exact original surface. Learning how scars develop and how treatments improve them helps people move toward clearer, healthier-looking skin.
Skin scarring forms when the body repairs damaged tissue after injury or inflammation. The skin quickly closes wounds, protecting deeper layers from infection and further damage. During this repair stage, the body produces collagen fibers that rebuild the injured area. Uneven collagen production often leaves visible marks, raised tissue, or shallow indentations.
Skin healing begins immediately after an injury, such as an acne lesion, cut, or burn. The body forms a blood clot that protects the damaged tissue and stops bleeding. Next, immune cells clean the wound and prepare the skin for rebuilding. Fibroblast cells then produce collagen, which helps reconnect the damaged layers of the skin. This collagen network strengthens the wound but rarely recreates the original skin structure. As a result, the repaired area may appear thicker, thinner, or uneven compared with the surrounding skin.
Skin scars appear in several forms depending on the depth of injury and the healing response. Atrophic scars create shallow depressions and often follow acne inflammation. Hypertrophic scars rise above the skin surface because excess collagen gathers in the healing area. Keloids grow beyond the original wound and form thick clusters of scar tissue. Burn injuries sometimes create contracture scars that tighten nearby skin and limit movement. Dermatologists use these scar categories to guide treatment selection and predict healing outcomes.
Several biological and environmental factors affect the development of skin scarring. Genetics influence how the body regulates collagen during tissue repair. Skin tone also affects scarring patterns because darker skin types develop keloids more frequently. Age affects the healing process because younger skin produces collagen more quickly. Additionally, infection or delayed treatment may worsen the appearance of the scar. Sun exposure during healing may darken scars and create uneven pigmentation.
The skin microbiome refers to the community of beneficial bacteria living on the skin surface. These microorganisms help regulate inflammation and protect the skin barrier during the healing process. When the microbiome becomes unbalanced after injury, irritation, and delayed repair may occur. Dermatology research increasingly links microbiome stability with healthier skin recovery and reduced scar formation.
Skin bacteria influence healing by controlling inflammation and protecting damaged tissue. Beneficial microbes help prevent harmful bacteria from entering wounds and causing infection. This protective activity allows skin cells to rebuild without excessive inflammation. When harsh products or antibiotics disrupt microbial balance, irritation may increase and slow the repair process. Dermatology studies show that balanced skin bacteria support stronger barrier function during healing. Healthy microbiome conditions often help scars fade more evenly as the skin rebuilds.
Healthy skincare habits help maintain the balance of beneficial skin bacteria. Gentle cleansers protect the skin barrier without stripping natural oils. Overuse of strong antibacterial products may disrupt the skin's microbial diversity. Dermatologists often recommend simple skincare routines during wound healing. This protective approach helps preserve the natural microbial environment that supports tissue repair. Balanced microbiome conditions may help reduce inflammation and promote smoother healing.
Reducing skin scarring begins with proper care during the healing stage. Gentle treatment supports healthy collagen production and balanced skin repair. Daily care habits protect fragile tissue and lower inflammation around the wound. Consistent attention during recovery often leads to smoother skin over time.

Proper wound care helps reduce skin scarring by supporting healthy tissue repair. Gently cleaning the wound removes bacteria and debris that may slow healing. Protective dressings maintain a moist environment, allowing new skin cells to regenerate efficiently. This protective care prevents cracking and irritation that can deepen scars. Avoid picking scabs because this habit disrupts the delicate rebuilding layers beneath. Dermatology guidance often confirms that consistent wound care improves healing outcomes and scar appearance.
Sun protection reduces discoloration that often appears during scar healing. Ultraviolet exposure stimulates excess pigment production in damaged skin. This pigment reaction may cause scars to appear darker than the surrounding tissue. Sunscreen with broad-spectrum protection shields healing skin from these effects. Protective clothing also reduces exposure to direct sunlight during recovery. Dermatology research shows that consistent sun protection helps scars fade more evenly.
A healthy diet strengthens the body's ability to repair damaged skin. Protein supplies amino acids that support collagen production during healing. Vitamin C helps stabilize newly formed collagen fibers and improve skin strength. Zinc also regulates inflammation and supports immune function during wound repair. Adequate hydration keeps skin cells active and maintains elasticity in healing tissue. Balanced nutrition supports steady skin recovery and healthier long-term texture.
Modern dermatology offers several treatments that improve the appearance of scars and skin texture. Some treatments target the skin's surface layers. Others stimulate collagen deeper within the tissue. Dermatologists often combine therapies to create greater improvements in scar appearance.
Topical treatments offer a noninvasive option for improving mild to moderate skin scarring. Silicone gels and silicone sheets remain widely recommended by dermatologists. These products hydrate scar tissue and regulate collagen buildup during healing. Retinoid creams may also improve skin texture by encouraging faster cell turnover. This treatment approach gradually softens scars and smooths uneven skin surfaces. Consistent application over several weeks usually produces the best visible improvement.
Microneedling improves skin scarring by stimulating natural collagen production. Dermatologists use fine needles to create controlled microchannels within the skin surface. These micro-injuries activate the body's repair response and increase collagen formation. New collagen gradually fills shallow depressions caused by acne scars. This treatment also improves skin elasticity and overall texture. Clinical dermatology data show that several sessions often deliver stronger results.
Laser therapy targets damaged skin layers using concentrated light energy. Dermatologists select different laser types based on scar depth and skin tone. Some lasers remove the outer damaged layer of skin to improve surface texture. Others reach deeper layers and stimulate collagen remodeling. This treatment may also reduce redness or uneven pigmentation around scars. Clinics often recommend multiple sessions for noticeable improvement.
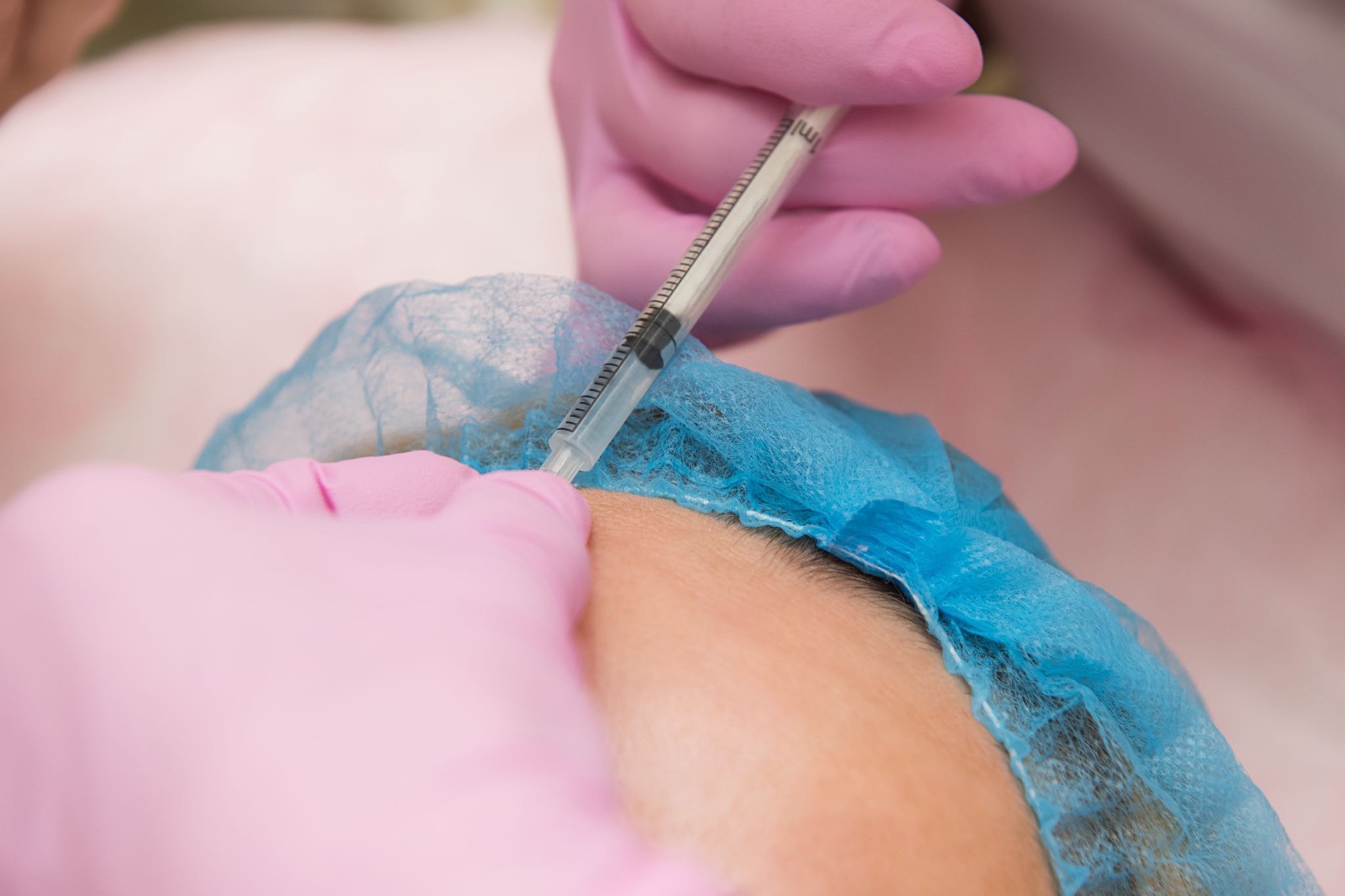
Injectable treatments reduce thick scar tissue that forms raised scars. Dermatologists commonly use corticosteroid injections to soften hypertrophic scars or keloids. These injections slow excess collagen production within the scar tissue. This medical treatment gradually flattens the raised scar surface. Doctors sometimes combine injections with laser therapy for greater improvement. Clinical dermatology practices report that combination treatments improve stubborn scars more effectively.
Healthy lifestyle habits support better healing and reduce the visibility of scars. Skin regeneration depends on balanced nutrition, rest, and consistent care. Small adjustments in daily routines influence inflammation and tissue repair. Over time, these habits contribute to smoother and healthier skin.
A gentle skincare routine supports healthy healing and protects sensitive tissue. Mild cleansers remove impurities without damaging the skin barrier. Hydrating moisturizers maintain skin flexibility and prevent dryness around scars. This protective hydration allows skin cells to rebuild more efficiently. Avoid harsh exfoliants or aggressive treatments during recovery. Dermatology experts often recommend simple routines to gradually improve the texture of scars.
Sleep supports skin regeneration and tissue repair throughout the night. During deep sleep, the body increases blood flow to the skin. This circulation delivers oxygen and nutrients to damaged tissue. Poor sleep habits increase inflammation and slow the healing process. Consistent rest also regulates hormones that influence skin health. Dermatology research continues to link quality sleep with improved healing outcomes.
Daily lifestyle choices influence how skin repairs itself after injury. Smoking restricts blood flow and reduces oxygen delivery to skin cells. This restriction slows collagen production and weakens tissue repair. Chronic stress may also increase inflammation and delay healing. Regular exercise improves circulation and supports healthy skin regeneration. Balanced habits create a healthier environment for skin recovery.
Hormones regulate many processes involved in skin repair and inflammation. These chemical messengers influence collagen production, oil levels, and immune responses during healing. Hormonal fluctuations may alter the rate of wound healing and the formation of scar tissue. Dermatology research increasingly recognizes hormonal balance as an important factor in skin recovery.
Hormones guide the body's response to injury and tissue rebuilding. Estrogen helps support collagen production and maintains skin elasticity during healing. Cortisol, a stress hormone, may increase inflammation when levels remain elevated for long periods. Increased inflammation can slow skin repair and contribute to thicker scars. Hormonal acne also causes repeated inflammation, which increases the risk of deeper acne scarring. Understanding these hormonal influences helps people connect overall health with visible skin outcomes.
Chronic stress affects the skin through hormonal changes. Elevated cortisol levels increase inflammation and weaken the skin's repair response. This inflammatory environment may slow wound healing and prolong redness around scars. Stress may also worsen acne outbreaks, which increases the likelihood of acne scarring. Dermatology studies increasingly connect emotional stress with delayed skin recovery. Managing stress through healthy routines can support better healing and improved skin texture.
Professional care often improves stubborn skin scarring that does not fade naturally. Dermatology specialists evaluate scar type, skin condition, and healing history before recommending treatment. This medical evaluation helps guide personalized plans that may include laser therapy, microneedling, injections, or targeted skincare. Clinics often base treatment decisions on clinical research and patient outcomes to improve safety and visible results. Long-term care supports collagen remodeling as scar tissue gradually changes beneath the skin. With consistent treatment and healthy skin habits, many people notice smoother texture and reduced scar visibility over time.
Visit the Naples Laser & Skin Aesthetics blog for trusted insights on skin treatments, scar care, and modern aesthetic solutions.
%402x.svg)

.png)
3641 10th St N Suite B, Naples, FL 34103